The content of this post was originally going to be included in the text on myths surrounding back pain (link to post), however because it is a somewhat complex topic and it will take some explanation to get my point across, it ended up developing into a topic worthy of its own text.
This time I’m looking at the myth of what is called ‘Text Neck’. Our necks are another part of our spine about which we have been given a lot of warnings. All over the internet there has been the clamouring for the recognition of this supposed condition, called “text-neck”. Just google it yourself – there are over 4 billion search results like it’s a very well-established thing.
Basically, like with the rest of our spine, we are told that flexing our neck, even though flexion is a natural movement of all parts of our spine, will cause either pain, injuries, or other health problems. So, the question here is: what is the actual relationship between a flexed neck, a forward head posture in clinical terminology, and pain in our neck?
One of the biggest and most recent studies about this is a systematic review and meta-analysis by Mahmoud et al (2019). They found 15 studies appropriate for review comparing measures of head and neck posture in people with and without neck pain. Most studies were of weak or moderate methodological quality (quality with which they are designed and executed) and there were a lot of differences between how head and neck posture was measured, which can make comparisons difficult and limits how sure we can be about the conclusions (Mahmoud et al, 2019). The authors found that there is an increase in forward head posture in adults with neck pain compared to adults without pain. However, there was no relevant difference between forward head posture in adolescents and adults over 50 years of age with or without neck pain.

So what gives? As a teenager, the age when we’re told that we’re always looking down at our phones, it doesn’t matter how you hold your neck, out of a sudden when you reach adulthood your neck posture starts giving you pain but that stops when you reach 50? I don’t know about you, but if the position is the problem, then this doesn’t make sense to me. Maybe your neck posture itself is not that relevant for having pain in your neck.
Considering that other studies looking at neck posture in adolescents do not show a relationship between static head posture, your posture when you’re not moving, and neck pain the authors hypothesize that this happens due to teenagers still being able to move their necks out of that flexed position and that what causes pain in adults is the loss of that ability (Mahmoud et al, 2019). The authors also theorize that the onset of pain as adults is related to loss of neck muscle endurance and flexibility as we age (Mahmoud et al, 2019).
There is still something here that doesn’t make sense. If we do assume that neck pain is caused by loss of range of movement of our neck, and this loss comes with age, why do we again stop seeing a link between neck posture and pain in those over 50 years of age?
I hope you’re starting to see how the research around this topic is not as straightforward as some people on the internet want us to believe.
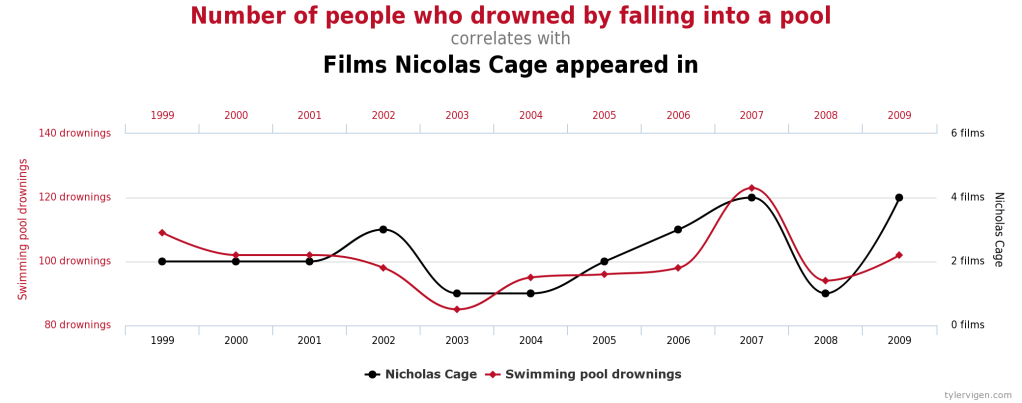
But there is also another detail that limits being able to say a certain posture causes neck pain. All the studies included by the authors in the review are cross-sectional (Mahmoud et al, 2019). This means they measure and analyse people at a single point in time and do not follow them up more over time. Because of this, this study design can’t find a relationship of causality. Who can assure us the reason they appeared with a flexed neck at that point in time wasn’t because they were in pain? Or that because they were being observed, that didn’t cause them to change how they hold their body to try to meet what they thought was the expectation of the examiners? We don’t know which one came first and this highlights the very important difference between correlation and causation.
Maybe it’s not about your posture. The association between neck pain and the amount of time we use our phones has also been looked at by Blumenberg et al (2021) and they did find that people who spent between 3 hours or more per day using their mobiles showed an increase prevalence of neck pain, as well as pain on other parts of the back. It’s important to note that they did not measure posture at rest, while using phones, or during activities.
So maybe it’s about making sure you get your joints to move often to keep them able to do so and keeping your muscles strong so they can actually move your joints. Maybe it’s about reducing the amount of time you spend in any one given posture, be it upright or flexed, sitting or standing.
How do you do that? You do it by reducing sedentary time and increasing your general amount of physical activity. Another thing to add to the benefits of exercise
But we meet the same problem again. Even though this study by Blumenberg et al (2021) used subjects from a study called the 1993 Pelotas birth cohort, which followed people from birth to when they were 22 years old, the authors only measured neck pain and total hours of use of mobile phones on the 22 years follow-up – this is, in a single point of pain. Thus, as identified by the authors, this data can only be considered cross-sectional (Blumenberg et al, 2021). To properly understand a causal relationship, we have to actually follow up people over multiple points in time and monitor the present, or lack thereof, of certain factors and their expected consequences. This is called a longitudinal design study. Luckily for us, there are a few recent studies looking exactly into that.
First, we have a study by Gustafsson et al (2017) focused on the topic of neck pain and mobile phone use. They started by examining 7092 people and the number of daily text massages. The authors managed to follow up with 4148 of those after 1 year, and again at 5 years with 2724 people from the original group (Gustafsson et al, 2017). They found that people who already had neck pain on initial assessment and were in the group with the highest reported number of daily texts, continued to have neck pain at 1-year follow-up, however, this association disappeared at 5 years (Gustafsson et al, 2017). In people without neck pain to start with, there was no correlation between developing neck pain at 1 or 5 years with any frequency of daily text messages (Gustafsson et al, 2017). One obvious limitation of this study is that they didn’t measure neck or head posture.
More recently we have the study produced by Richards et al (2021) which used the group of 2868 participants originally followed by the Raine Study who were enrolled in 1989, at around their 18th week of gestation – yes while still in the womb – and the followed-up in regular intervals. The good thing about this study is that they actually assessed neck posture, as well as neck pain, and at two different points in time: when participants were 17 years old and again at 22 years old. Let’s quickly go through their findings. Having neck pain at 17 was associated with having neck pain at 22, independently of other factors. So if you have neck pain when you are younger, you are more likely to still have it when you are older. But now comes the interesting part. In male participants, there did not appear to be any particular factors that strongly correlated to having or not having neck pain, but there was one such factor in females: compared with having an upright posture, having a slumped or flexed posture appears to decrease the risk of having neck pain when participants became 22 years old. So, if you’re female, having a more rounded, head forward posture will reduce your chances of having neck pain at 22 years of age, but not if you’re a male? How do we make sense of this information?

Well, maybe it indicates that your posture is not a significant factor in the development, or not, of neck pain. I hope I have been able to demonstrate that across the biggest and best-designed studies, like with back pain (link to post), we cannot find a causal relationship between our neck and head posture, nor the amount of texting we do on our phones and the risk of developing neck pain. We see that people can present with flexed postures, however, we can’t say that isn’t a consequence of pain instead of the other way around. And in some cases, a flexed posture even seems to lead to less pain.
Am I safe to say R.I.P to the myth of ‘text neck’ and ask that we please stop making up new diagnoses or diseases without sufficient data to back them up? As soon as another non-evidence-based belief is made up, it easily gets widely spread by all forms of media around us (Slater et al., 2019), contributing to people believing it is a thing when it isn’t. Misinformation is really easy to spread, particularly in a society where critical thinking often isn’t promoted or rewarded.
Don’t be afraid to flex your spine, it is made to move. And don’t be afraid to read or be on your phone, at least not due to fear of it damaging your neck. Your body is more resilient than that. But don’t forget to also be active and get some exercise in. That’s how you ensure your joints remain healthy and able to move, amongst many other benefits.
Thank you for reading through and as always, if you learned something and/or found this text interesting, please share it all over social media so you can help others learn. See you in the next one.
References:
Blumenberg, C., Wehrmeister, F. C., Barros, F. C., Flesch, B. D., Guimarães, F., Valério, I., Ferreira, L. Z., Echeverria, M., Karam, S. A., Gonçalves, H., & Menezes, A. M. B. (2021). Association of the length of time using computers and mobile devices with low back, neck and mid-back pains: findings from a birth cohort. Public Health, 195, 1–6. https://doi.org/10.1016/j.puhe.2021.04.003
Christe, G., Nzamba, J., Desarzens, L., Leuba, A., Darlow, B. and Pichonnaz, C. 2021. Physiotherapists’ attitudes and beliefs about low back pain influence their clinical decisions and advice, Musculoskeletal Science and Practice. Elsevier Ltd, 53(April), p. 102382. doi: 10.1016/j.msksp.2021.102382.
Christe, G., Pizzolato, V., Meyer, M., Nzamba, J. and Pichonnaz, C. 2021. Unhelpful beliefs and attitudes about low back pain in the general population: A cross-sectional survey. Musculoskeletal Science and Practice. Elsevier Ltd, 52(August 2020), p. 102342. doi: 10.1016/j.msksp.2021.102342.
Foster, N. E., Anema, J. R., Cherkin, D., Chou, R., Cohen, S. P., Gross, D. P., Ferreira, P. H., Fritz, J. M., Koes, B. W., Peul, W., Turner, J. A., Maher, C. G. (2018). Prevention and treatment of low back pain: evidence, challenges, and promising directions. In The Lancet (Vol. 391, Issue 10137, pp. 2368–2383). Lancet Publishing Group. https://doi.org/10.1016/S0140-6736(18)30489-6
Gustafsson, E., Thomée, S., Grimby-Ekman, A., & Hagberg, M. (2017). Texting on mobile phones and musculoskeletal disorders in young adults: A five-year cohort study. Applied Ergonomics, 58, 208–214. https://doi.org/10.1016/j.apergo.2016.06.012
Korakakis, V., O’Sullivan, K., O’Sullivan, P. B., Evagelinou, V., Sotiralis, Y., Sideris, A., Sakellariou, K., Karanasios, S., & Giakas, G. (2019). Physiotherapist perceptions of optimal sitting and standing posture. Musculoskeletal Science and Practice, 39, 24–31. https://doi.org/10.1016/j.msksp.2018.11.004
Laird, R. A., Kent, P., & Keating, J. L. (2012). Modifying patterns of movement in people with low back pain -does it help? A systematic review. In BMC Musculoskeletal Disorders (Vol. 13). BioMed Central Ltd. https://doi.org/10.1186/1471-2474-13-169
Lima, M., Ferreira, A. S., Reis, F. J. J., Paes, V., & Meziat-Filho, N. (2018). Chronic low back pain and back muscle activity during functional tasks. Gait and Posture, 61, 250–256. https://doi.org/10.1016/j.gaitpost.2018.01.021
Mahmoud, N. F., Hassan, K. A., Abdelmajeed, S. F., Moustafa, I. M., & Silva, A. G. (2019). The Relationship Between Forward Head Posture and Neck Pain: a Systematic Review and Meta-Analysis. In Current Reviews in Musculoskeletal Medicine (Vol. 12, Issue 4, pp. 562–577). Springer. https://doi.org/10.1007/s12178-019-09594-y
Richards, K. v., Beales, D. J., Smith, A. L., O’sullivan, P. B., & Straker, L. M. (2021). Is neck posture subgroup in late adolescence a risk factor for persistent neck pain in young adults? a prospective study. Physical Therapy, 101(3). https://doi.org/10.1093/ptj/pzab007
Sheha, E. D., Steinhaus, M. E., Kim, H. J., Cunningham, M. E., Fragomen, A. T., & Rozbruch, S. R. (2018). Leg-Length Discrepancy, Functional Scoliosis, and Low Back Pain. In JBJS reviews (Vol. 6, Issue 8, p. e6). NLM (Medline). https://doi.org/10.2106/JBJS.RVW.17.00148
Slater, D., Korakakis, V., O’Sullivan, P., Nolan, D., & O’Sullivan, K. (2019). “Sit up straight”: Time to Re-evaluate. In Journal of Orthopaedic and Sports Physical Therapy (Vol. 49, Issue 8, pp. 562–564). Movement Science Media. https://doi.org/10.2519/jospt.2019.0610